Tuberculosis (TB)
 Tuberculosis (TB) is a disease caused by Mycobacterium tuberculosis, a germ that is spread from person to person through the air. TB usually affects the lungs, but it can also affect other parts of the body, such as the brain, the kidneys, or the spine. A person with TB disease can die if they do not get treatment.
Tuberculosis (TB) is a disease caused by Mycobacterium tuberculosis, a germ that is spread from person to person through the air. TB usually affects the lungs, but it can also affect other parts of the body, such as the brain, the kidneys, or the spine. A person with TB disease can die if they do not get treatment.
TB disease can be cured with medical care and the right medicine. Learn more...
Recent News
- DSHS TB Medication Availability Notification: April 9, 2024
- TB Standing Delegation Orders and Standing Medical Orders
- Enroll in Medicaid as a TB Medical Provider
Quick Links
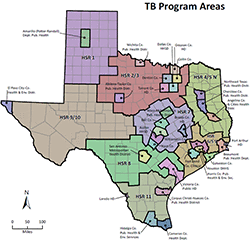 TB Public Health Program Contacts in Texas
TB Public Health Program Contacts in Texas- DSHS Mycobacteriology Laboratory
- DSHS Pharmacy
- Texas Center for Infectious Disease (TCID)
- Regional & Local Health Operations (RLHO)
- National TB Controllers Association
- Heartland National TB Center
- CDC Tuberculosis (TB)
- TAC Title 25 Part 1 Chap. 97
- Health & Safety Code Chap. 81
- Health & Safety Code Chap. 89








